Automated Billing for Mental Health Practices
Stop losing evenings to billing work
When a session wraps up, billing should keep moving. TheraNest’s therapy billing software automates invoicing, claim submission, and payment posting so routine billing runs without you and exceptions surface in one place when a human decision is actually needed.
What automation changes about your week
Most billing errors aren’t caused by complexity, they’re caused by repetition. The same steps, done manually, hundreds of times a month. TheraNest automates the routine so your team focuses on exceptions, not execution.
TheraNest handles billing for clinicians with different license types, rates, and payer credentialing. Whether you’re billing under a supervising clinician or managing a group practice with varied specialties, the system tracks who rendered the service and bills accordingly.
Resubmission is more expensive than submission. TheraNest checks claims against your payer rules before they go out, flagging common rejection triggers at the source, not three weeks later when a denial lands in your queue.
Automation doesn’t mean losing oversight. Choose which payers, plan types, or clinicians to automate first. Review claims before submission if you prefer. Every action is logged, and anything outside your defined rules surfaces to a single exceptions queue for human review.
From session to payment, automatically
Tell TheraNest how your payers, plan types, modifiers, and exceptions work. We can help you set this up during onboarding so you’re not guessing at payer-specific preferences or requirements.
Once configured, the system follows your billing preferences. You don’t re-enter this for every claim.

For eligible appointments, TheraNest creates the invoice, prepares the claim, and submits it automatically. When payment comes back, ERA posting applies it to the right claim without manual work. No missed charges. No unbilled batches sitting at the end of the week.

Automation handles the routine. Anything outside your rules, like an unusual payer response, a claim that needs review, or an ERA that doesn’t match, appears in a single exceptions queue. No hunting across screens.

Every claim, ERA, and payment adjustment is logged and linked to the original appointment. If a payer requests documentation or you run an internal audit, the full billing history is organized and accessible. No need to reconstruct records from memory.

Automate your billing workflow as your practice grows. Explore pricing plans.
Real results from real users
What’s your billing time really worth?
Most therapists who automate billing don’t stop thinking about it overnight. If you’d rather see the billing workflow in action before committing, we’ll walk you through it live.
Frequently Asked Questions
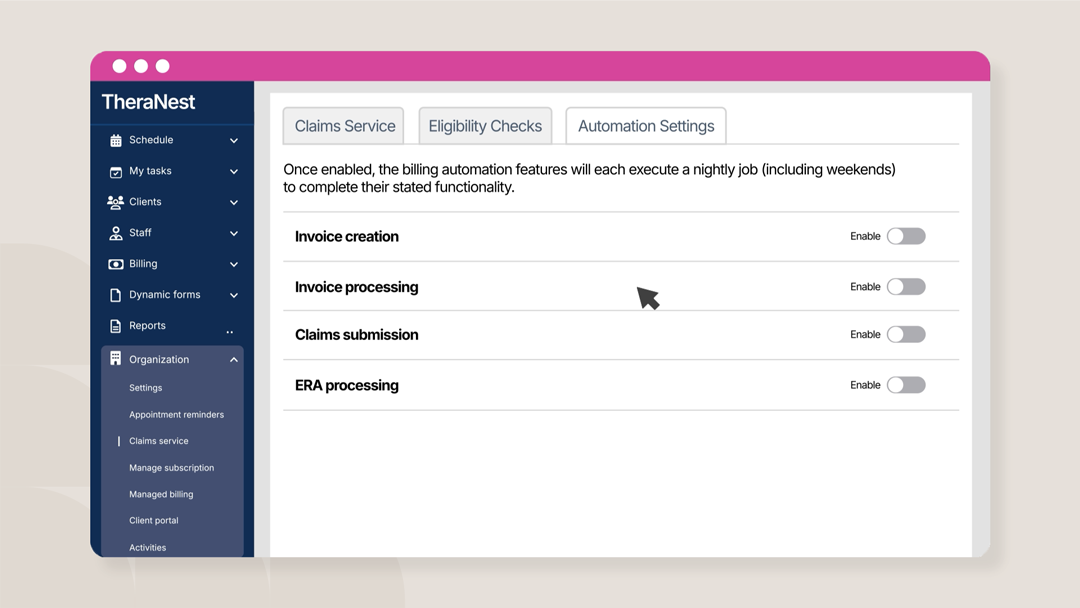
- Invoice creation for new appointments, or for appointments whose clinical documentation is newly signed.
- Invoice processing, which prepares the claims for submission.
- Claim submission, which transmits claims to the payers.
- ERA processing, auto-post ERAs according to your posting rules, or block them from posting if they meet certain conditions.
For example, if certain clinicians at your practice should always bill under the practice’s Type 2 NPI for a specific payer – rather than under their own – you can set a rule that blocks auto-submission whenever that payer and billing provider combination appears on a claim. The claim is held for review rather than submitted, so your billing team can correct the NPI before it goes out. Rules can be configured by primary insurer, billing provider, rendering provider, or service type, and combinations of those.
Your billing team can track claim statuses across all clinicians in Claims Manager and focus on the items that need attention, while routine claims keep moving on schedule.


